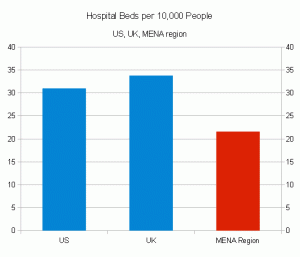
MENA health infrastructure remains underdeveloped despite the region's strong growth potential.
The Middle East & North Africa (MENA) region’s healthcare sector is growing, driven by larger populations, longer life expectancy and rising income. Still, MENA healthcare remains underdeveloped compared to western countries, according to a recent report from Al Masah Capital.
About 214 million people currently live in the MENA region, and that number is expected to swell to 272 million by 2025. Life expectancy has risen from 59 to 71 over the last 30 years, and infant mortality has fallen from 90 per 1,000 live births to 26.
As populations have grown income has also risen, from an average $3,727 per person to $8,187 over the last decade. This, combined with countries’ increasing readiness to use private medical insurance to fund health expenditure, has brought mandatory health insurance laws to Saudi Arabia, Abu Dhabi and Kuwait. It has also led expat-heavy GCC countries to scale back government coverage for foreigners. In Dubai, for example, expats are no longer eligible for free cancer treatment.
Though the region’s demographics bode well for the development of its healthcare sector, Al Masah found existing health infrastructure inadequate. The average number of hospital beds is only 21.6 per 10,000, compared to 33.8 in the UK and 31.0 in the US. Medical personnel are also lacking, with 79% fewer dentists and 71% fewer nurses than the US.
Report author Shailesh Dash said:
Statistics show that there are spikes in some medical conditions peculiar to this region. Prevalence of non-communicable or lifestyle diseases such as diabetes, cardiovascular ailments and certain forms of cancer are rising. The International Diabetes Federation estimates that the number of people suffering from diabetes in the MENA region is set to nearly double to 51.7 million by 2030 from 26.6 million currently. This is a sobering thought and demands a warfront footing to combat.
Dash envisioned the private sector as the solution, arguing it will be able to develop the region’s health infrastructure while easing the cost burden on governments. “The US government, used as a benchmark, bears less than 50% of the total healthcare costs in the economy,” he noted, “compared to 64% in the MENA.”
Dash should be leery of using the US as a benchmark, however. While the US government may spend less on healthcare, the percentage of US GDP devoted to healthcare is significantly higher than in other developed countries, pointing to severe cost inefficiencies. Hence, while the MENA region certainly offers vast potential for the private sector, large-scale privatization a la the US is unlikely the best way of ensuring quality healthcare for the majority of the population.
